Ever looked at your MRI report and seen the phrase “thecal sac compression” without really understanding what it means for your daily life?
Most people focus on the scary-sounding medical terms while missing the bigger picture. This condition shows up on countless spine scans every day, but the real question isn’t just about what appears on imaging.
What matters most is how this compression affects your body, which warning signs require immediate attention, and when conservative care is no longer enough.
Some people live with mild compression and barely notice it. Others experience serious neurological changes that require prompt action.
The difference lies in recognizing specific patterns, understanding what your body is telling you, and knowing exactly when to seek help. Let’s break down everything you need to know.
What Is Thecal Sac Compression?
Thecal sac compression is a spinal condition that affects the protective membrane surrounding your spinal cord and nerve roots.
The spinal cord and peripheral nervous system work together to transmit signals between your brain and body. Understanding basic spine anatomy helps you grasp what compression means for your health.
Think of your spine as a main highway where nerve signals travel between your brain and body. Thecal sac compression creates a “traffic jam” that disrupts this crucial communication system.
The dural sac, also known as the thecal sac, is a fluid-filled protective covering that cushions your spinal cord within the spinal canal.
When this sac becomes flattened or compressed against the spinal cord, it can interfere with your brain’s ability to send and receive messages from different parts of your body.
What Causes Thecal Sac Compression?
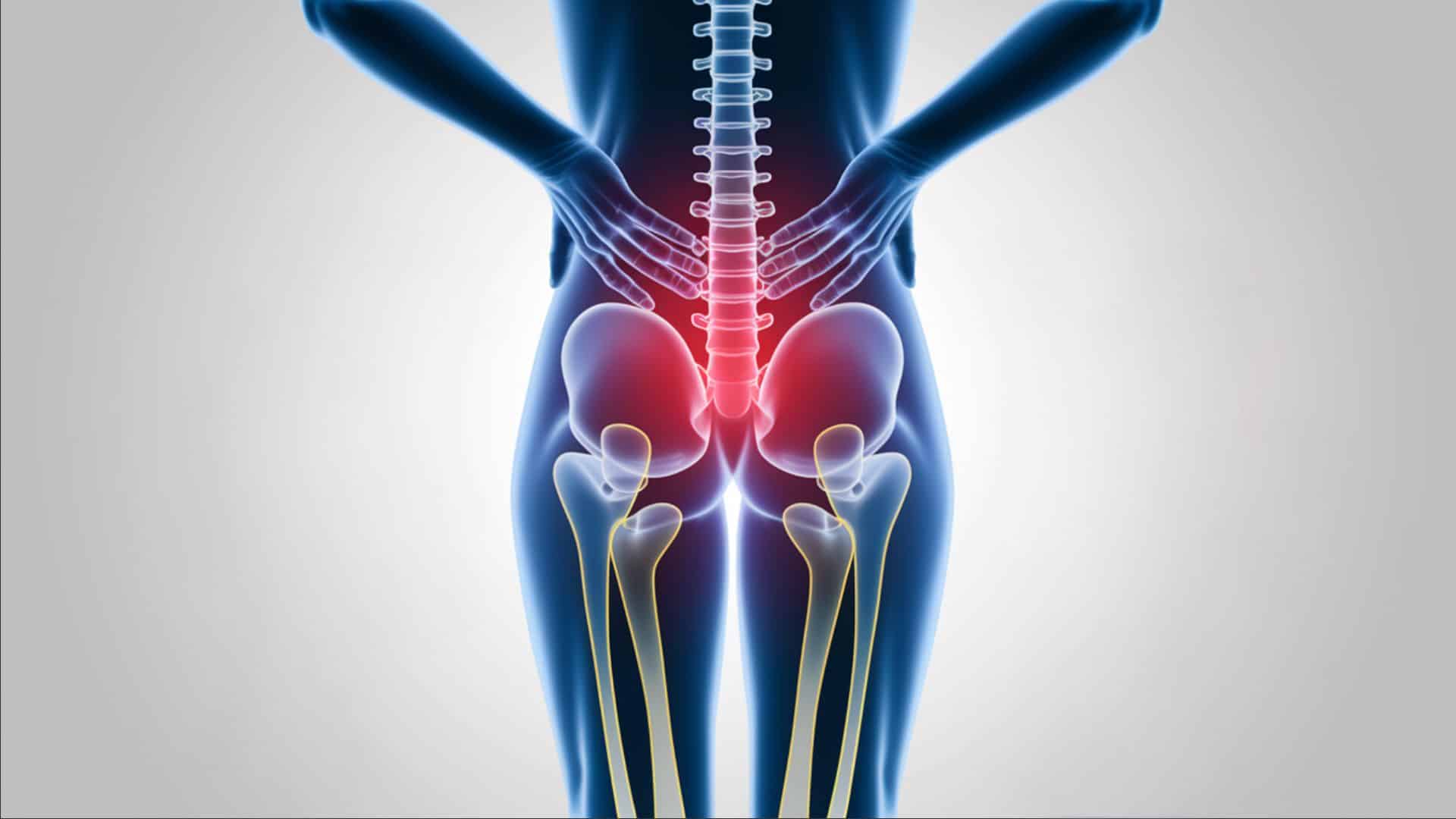
Several spine problems can push against the thecal sac. Here are the most common causes, starting with what doctors see most often.
- Herniated or bulging discs: The soft cushion between the spine bones bulges out. This bulge takes up space in the spinal canal. It pushes directly against the thecal sac.
- Spinal stenosis: This narrows the canal where nerves travel. Bone spurs, thickened ligaments, and arthritis reduce the available space.
- Degenerative disc disease: It causes discs to flatten and lose height. The spine bones move closer together. This change can pinch nerves and compress the protective covering.
- Arthritis: This creates bone overgrowth. These extra bone formations jut into the spinal canal. They reduce space and press on the sac.
- Spondylolisthesis: This happens when one vertebra slips forward over another. The misalignment narrows the canal. This creates pressure on the nerves inside the sac.
Less common causes include spinal tumors, which can grow inside or near the canal. Trauma from accidents may cause fractures or swelling that compresses nerves. Infections rarely cause abscesses that press on the sac.
Thecal Sac Compression Symptoms

Thecal sac compression symptoms vary depending on where the pressure is and how severe it is. Most people notice certain warning signs first.
- Pain: usually the earliest symptom. It may start in your back or neck. The discomfort often spreads down your arms or legs. Some describe it as sharp, while others feel a dull ache.
- Numbness and tingling: happen when nerves get irritated. You might feel pins and needles in your hands, feet, or limbs. These sensations may come and go at first.
- Weakness: develops when nerve signals can’t travel properly. Muscles don’t receive full instructions from your brain. You might struggle to grip objects or lift your foot.
- Limited range of motion: makes bending or turning harder. Your spine feels stiff. Certain movements trigger sharp pain or increase numbness.
- Walking difficulties: they appear when leg nerves are affected. Your legs may feel heavy or uncoordinated. Some people develop a limp or shuffle their feet.
- Radiating pain: shoots down specific nerve paths. If your lower back is compressed, pain may travel down your buttocks and leg. This is often called sciatica.
- Balance problems: they occur when sensory nerves are compressed. You might feel unsteady on your feet. Stairs become more challenging.
Not everyone experiences all symptoms. Some people have mostly pain. Others deal with numbness or weakness as the main issue.
Ignoring these signs can lead to severe, debilitating pain and even permanent neurological damage. Early detection through medical evaluation and imaging tests like MRIs can prevent minor issues from becoming major, life-altering conditions.
Thecal Sac Compression Symptoms by Spine Location
Where compression happens determines which thecal sac compression symptoms you feel. Each spine region controls different body areas. Understanding these patterns helps you describe your symptoms to doctors.
1. Cervical (C-Spine) Symptoms
Neck compression (cervical spine) can affect your arms, hands, and sometimes your legs.
- Neck pain: Radiates to the shoulders or between the shoulder blades; worse with turning the head.
- Arm numbness/tingling: Follows nerve patterns: C5 shoulder, C6 thumb/index, C7 middle finger, C8 ring/pinky.
- Hand weakness: Poor grip, frequent dropping, difficulty with buttons or jars.
- Coordination issues (myelopathy): Clumsy hands and trouble with fine motor tasks like writing.
- Leg symptoms: Stiffness, weakness, or awkward walking from severe spinal cord compression.
- Bowel/bladder changes: Rare but urgent red flag needing immediate medical attention.
2. Lumbar (L-Spine) Symptoms
Lower back (lumbar) compression is the most common location. Symptoms affect your legs, feet, and lower body.
- Lower back pain: Often the first symptom; worsens with prolonged sitting or standing.
- Sciatica: Sharp pain radiating down the buttock and leg, usually worse on one side.
- Leg numbness: Dermatomal pattern: L4 inner thigh/shin, L5 top of foot/big toe, S1 outer foot/small toes.
- Foot weakness: L5/S1 compression causing foot drop, tripping, or dragging the foot.
- Walking intolerance: Leg heaviness, numbness, or fatigue with walking, relieved by sitting or leaning forward.
- Saddle numbness: Loss of sensation in the groin, buttocks, and inner thighs is an emergency sign.
- Bowel/bladder dysfunction: Loss of control or sensation indicates a medical emergency.
3. Thoracic (T-Spine) Symptoms
Mid-back (thoracic) compression is less common but creates unique symptoms.
- Band-like tightness: Wraps around the torso, often described as a tight belt or band.
- Chest/abdominal pain: Follows rib nerve paths and may mimic heart or digestive issues.
- Balance problems: Unsteady walking due to disrupted leg sensory signals, worse on uneven ground.
- Leg stiffness/weakness: Heavy, hard-to-control legs indicate spinal cord compression.
- Electric shock sensation: Shock-like feeling down the spine with neck movement, signaling cord involvement.
While symptoms vary based on where compression occurs in the spine, their intensity and functional impact are best understood by how severe the compression becomes.
Thecal Sac Compression Symptoms by Severity
Thecal sac compression symptoms often progress over time. Understanding these stages helps you know when to seek care.
| Severity | Key Features (Very Concise) |
|---|---|
| Mild | Intermittent pain, brief numbness/tingling, no weakness, full motion, symptoms improve with rest and conservative care |
| Moderate | Daily persistent pain, constant numbness, mild–moderate weakness, reduced walking tolerance, sleep disruption, needs medical evaluation |
| Severe | Marked weakness, muscle atrophy, reflex loss, abnormal gait, severe pain, bowel/bladder issues, worsening despite care; often needs surgery |
Symptoms often progress from mild to severe: worsening pain, weakness, or bowel/bladder changes signal the need for urgent medical evaluation.
Emergency Symptoms (When to Seek Immediate Care)
Some thecal sac compression symptoms require urgent medical attention. Cauda equina syndrome is the most critical emergency. This happens when nerves at the base of your spine get severely compressed.
Watch for these warning signs:
- Saddle anesthesia
- Bowel dysfunction
- Bladder dysfunction
- Bilateral leg weakness
- Sexual dysfunction
- Rapidly worsening symptoms
Other urgent situations include severe myelopathy signs, complete foot drop, fever with back pain, and trauma.
If you experience any of these symptoms, go to the emergency room immediately. Don’t wait for a regular doctor appointment. These conditions can cause permanent nerve damage if not treated quickly.
Early intervention (usually within 24-48 hours) gives the best chance for full recovery. Delays can result in lasting disability.
How Does Thecal Sac Compression Disrupt Daily Life?

Living with untreated thecal sac compression can feel like carrying an invisible burden that affects every aspect of your life.
What starts as minor difficulties can progressively become severe and debilitating, impacting work, relationships, and overall well-being.
1. Work Performance Decline
Concentration wanes as constant discomfort takes its toll. Frequent medical appointments and pain-related absences become common, affecting productivity and professional relationships. Tasks that once seemed effortless now require significant effort and planning.
2. Physical Activity Limitations
Simple activities like standing for extended periods or lifting everyday objects become challenging. Walking without pain becomes uncertain, and participation in previously enjoyed physical activities may need to be avoided entirely.
3. Social Withdrawal
The invisible burden of chronic pain leads to avoiding friends and family gatherings. Social isolation increases as leaving the house or engaging in group activities becomes too uncomfortable or unpredictable.
4. Sleep Disruption
Finding comfortable sleeping positions becomes difficult, leading to poor sleep quality. Restless nights compound daytime fatigue and pain, creating a cycle that affects overall well-being and recovery.
5. Emotional Impact
Living with constant uncertainty about daily functioning creates frustration and anxiety. The emotional toll of dealing with chronic discomfort affects mental health, relationships, and overall quality of life significantly.
As symptoms begin to interfere with daily function and quality of life, treatment shifts from understanding the impact to exploring options that relieve pressure and prevent permanent nerve damage.
Treatment Options for Thecal Sac Compression
Treatment for thecal sac compression follows a progressive approach, starting with conservative methods and advancing to surgical interventions when symptoms persist or worsen.
The American Physical Therapy Association recommends working with spine specialists who design personalized exercise programs. Proper guidance prevents exercises that might worsen compression.
| Conservative Treatments | Surgical Solutions |
|---|---|
| First Line of Defense | When Conservative Care Isn’t Enough |
| Physical therapy | Microsurgery |
| Posture correction & ergonomics | Interspinous process decompression |
| Anti-inflammatory medications | Percutaneous discectomy/foraminotomy |
| Steroid injections | |
| Holistic health integration | |
| Goals | Goals |
| Manage symptoms | Relieve nerve pressure |
| Strengthen supporting muscles | Prevent progression |
| Reduce inflammation | Restore function |
| Address root causes | Emergency intervention |
| Best For | Best For |
| Early-stage compression | Severe neurological issues |
| Mild to moderate symptoms | Failed conservative treatment |
| Prevention-focused care | Risk of permanent damage |
Early intervention with conservative treatments can effectively manage most cases, but surgical options become necessary when non-surgical methods fail to prevent permanent neurological damage.
Act Early for a Better Outcome:
Early intervention is crucial because thecal sac compression can rapidly progress from minor discomfort to permanent neurological damage. Delaying treatment risks developing cauda equina syndrome, potentially causing paralysis or incontinence.
When Surgery Is Clearly Indicated for Thecal Sac Compression
Surgery for thecal sac compression symptoms becomes necessary in specific situations. These criteria help doctors decide when conservative treatment isn’t enough.
| Surgical Indication | Key Points |
|---|---|
| Cauda equina syndrome | Bowel loss, saddle numbness, bilateral leg weakness, and sexual dysfunction |
| Progressive weakness | Worsening foot drop, grip loss, trouble standing → nerve damage risk |
| Severe myelopathy | Clumsy hands, gait/balance issues, spastic legs, poor coordination |
| Failed conservative care | No improvement after 6-12 weeks of PT/meds/injections |
| Intolerable pain | Pain prevents work, sleep, or basic function |
| Major functional limits | Can’t work, self-care, walk distances, or perform daily activities |
| Non-conservative pathology | Severe stenosis, large disc herniation, spondylolisthesis, tumor/cyst |
Most importantly, surgery addresses the compression but doesn’t cure underlying spine problems. Post-surgical rehabilitation and lifestyle modifications remain important for long-term success.
Remember, you are your best advocate. Understanding your condition and treatment options helps you participate actively in your care.
Conclusion
Thecal sac compression symptoms range from mild discomfort to serious neurological emergencies. The key is knowing which category your situation falls into.
Most cases respond well to physical therapy, medication, and lifestyle changes over 6-12 weeks. However, red flags like bowel changes, saddle numbness, or rapidly progressing weakness require immediate emergency care.
Don’t panic if your MRI shows compression, but don’t ignore worsening symptoms either. Track your symptoms daily, follow your treatment plan consistently, and maintain open communication with your doctor.
If conservative treatment isn’t helping after a reasonable trial, discuss other options. Early intervention prevents permanent nerve damage.
Schedule that appointment, ask the right questions, and take control of your spine health today. Take the next step in healing. Visit our Recovery & Wellness hub for expert-driven guidance.
Frequently Asked Questions
What Kind of Doctor Treats Thecal Sac Compression?
Orthopedic spine surgeons, neurosurgeons, or physiatrists typically treat this condition. Start with your primary care doctor for referrals to the appropriate specialist based on severity.
What Should I Avoid with Thecal Sac Compression?
Avoid heavy lifting, prolonged sitting, high-impact activities, and forward bending. Skip exercises that worsen pain. Stop smoking and maintain a healthy weight for better spine health.
Can Thecal Sac Compression Heal on Its Own?
Mild compression may improve with conservative treatment like physical therapy and rest. However, moderate to severe cases rarely resolve without intervention. Progressive symptoms require treatment.
Can a Ct Scan Show a Pinched Nerve?
CT scans show bone details but miss soft tissue like nerves. MRI remains better for pinched nerves. CT myelogram with contrast reveals nerve compression clearly.