No, CRPS does not directly shorten your life expectancy. Research confirms that Complex Regional Pain Syndrome itself is not a life-threatening condition, and most patients have a normal lifespan.
However, secondary health complications from chronic pain, immobility, and untreated mental health conditions can create real risks that deserve serious attention.
This article breaks down exactly what the research shows, which secondary risks actually matter, and specific steps you can take to protect your long-term health.
What Is CRPS? A One-Sentence Overview
Complex Regional Pain Syndrome is a chronic pain disorder affecting the nervous system after an injury or surgery.
Key Facts About CRPS:
- Pain is out of proportion to the severity of the initial injury
- Most commonly affects your arm, leg, hand, or foot
- Pain signals don’t shut off even after your injury heals
CRPS involves the peripheral and central nervous systems and can progress unpredictably. Early diagnosis and treatment improve outcomes.
Now that you know what CRPS is, let’s address the question that worries most patients and families.
What the Research Actually Shows About CRPS and Lifespan
Complex Regional Pain Syndrome is a chronic neurological condition causing severe pain, typically in a limb, following injury or surgery.
CRPS Mortality Rate: The Medical Consensus
Multiple peer-reviewed studies confirm CRPS does not directly reduce life expectancy:
- A 2022 systematic review published in the European Journal of Pain by Groeneweg et al. found no evidence that CRPS itself shortens lifespan. The study analyzed 22 cohorts and concluded that while pain and motor dysfunction persist in 51%–89% of patients beyond 12 months, mortality rates were not elevated compared to the general population.
- According to the National Institute of Neurological Disorders and Stroke (NINDS), CRPS is not classified as a life-threatening condition, though severe cases can cause significant disability.
- Cleveland Clinic’s pain medicine department states that, with proper management, most people with CRPS can live long, fulfilling lives.
Why There Is No Fixed CRPS Life Expectancy Number
There’s no single answer because CRPS affects everyone differently:
- Disease severity varies significantly between patients
- Some recover within months, while others experience symptoms for years
- The Groeneweg et al. (2022) review found grip strength reduced by 25%–66% and range of motion reduced by 20%–25% at 12+ months, but these functional impacts don’t correlate with mortality
The real concern isn’t CRPS itself; it’s the secondary health problems that can develop from chronic pain and limited mobility.
Secondary Health Risks That Can Shorten Life Expectancy in CRPS
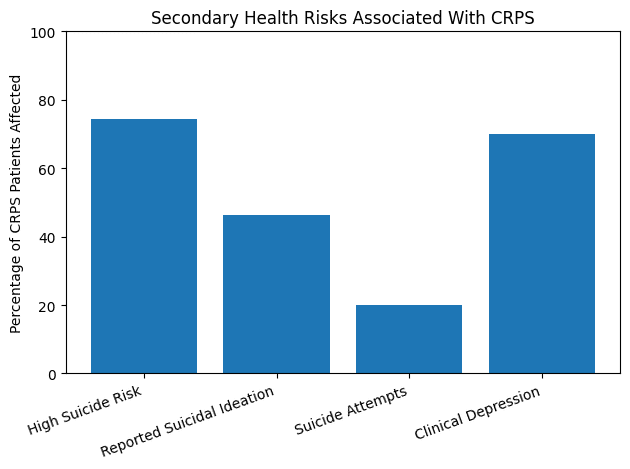
While CRPS won’t kill you directly, the ripple effects it creates can be dangerous. Here’s what the research shows about each risk:
CRPS and Suicide Risk: The Most Critical Factor
Suicide risk is significantly elevated in CRPS patients:
- A 2014 study by Lee et al. published in Psychiatry Investigation found that 74.4% of CRPS patients were at high risk for suicidal ideation
- A web-based epidemiological survey found that 46.4% of CRPS-1 patients reported experiencing suicidal ideation, and 20% had attempted suicide
- Risk factors significantly associated with suicidal ideation include depression (p=0.002), severity of pain (p=0.024), and decreased functioning (p=0.027)
Depression rates are exceptionally high:
- Approximately 70% of CRPS patients qualify for a diagnosis of depressive disorder according to structured clinical interviews
- More than 80% of patients in the Lee et al. study had been treated with antidepressants
CRPS and Heart Disease: Cardiovascular and Metabolic Risks
Immobility from CRPS creates cascading health problems:
- Stanford University research indicates CRPS can cause autonomic dysfunction, leading to rapid heart rate, blood pressure fluctuations, and poor circulation
- Increased heart rate and decreased heart rate variability observed in CRPS patients suggest autonomic imbalance, an independent predictor for increased mortality risk
- A sedentary lifestyle leads to weight gain, increasing the risk of heart disease, diabetes, and hypertension
CRPS Medication Side Effects and Long-Term Dangers
Long-term pain management carries its own risks:
- Polypharmacy increases fall and mortality risk, particularly in older patients
- Chronic opioid use can cause respiratory depression, liver damage, and dependency
- Drug interactions become more likely as treatment complexity increases
Severe CRPS Disability Complications
Physical deterioration creates additional health threats:
- Muscle atrophy and bone density loss increase fracture risk
- Skin breakdown and ulcers can lead to serious infections
- Joint contractures may become irreversible if left untreated
CRPS Prognosis: Factors That Improve or Worsen Your Outcome
Your prognosis with CRPS isn’t random. Research has identified specific factors that influence long-term outcomes:
Risk Factors for Poor CRPS Prognosis
| Factor | Impact |
|---|---|
| Delayed diagnosis | The mean diagnostic delay of 2.8 years leads to disease progression and worse disability |
| High baseline pain | Intense early pain strongly predicts poor long-term outcomes and work disability |
| Untreated mental health | Anxiety and depression at baseline predict worse pain and disability 8 years later |
| Smoking | Multiple studies show smoking worsens prognosis and slows recovery |
Factors That Improve CRPS Recovery and Long-Term Outcomes
| Factor | Impact |
|---|---|
| Early multidisciplinary care | Treatment started early allows improvement and even remission (Mayo Clinic) |
| Consistent movement | Exercise within tolerance prevents muscle wasting and maintains function |
| Integrated mental health support | Therapy combined with strong social/family support improves recovery rates |
| Younger age | Children, adolescents, and healthy younger adults show better recovery rates |
What Pain Specialists Say About CRPS Life Expectancy?
“The most important goals are to relieve pain and restore movement and strength in the affected limb. By achieving pain relief, you increase the odds of improving function and quality of life.”
The medical consensus is clear: CRPS itself is not life-threatening, but comprehensive care addressing both physical and mental health is essential for protecting long-term well-being.
How to Protect Long-Term Health With CRPS: Monitoring Checklist
Proactive monitoring and care can catch problems early and prevent serious complications.
Essential Health Screenings for CRPS Patients
Cardiovascular monitoring (annually): Autonomic dysfunction in CRPS can affect heart function. Request heart rate variability testing and blood pressure monitoring, especially if you notice rapid heartbeat or circulation changes.
Mental health assessments (every 3–6 months): Given that up to 70% of CRPS patients experience depression, regular mental health check-ins are essential, not optional. Don’t wait for a crisis.
Medication reviews (annually): Check for drug interactions, side effects, and whether each medication remains necessary. Discuss alternatives if side effects are impacting your quality of life.
Bone density scans (as needed): CRPS-affected limbs often show bone density loss due to immobility. If your mobility is significantly limited, request a DEXA scan to assess fracture risk.
Weekly CRPS Symptom Tracking Checklist
Monitor these indicators and share patterns with your healthcare team:
- Activity tolerance (are you able to do more or less than last week?)
- Sleep quality and total hours
- Mood changes (sadness, anxiety, hopelessness, irritability)
- Medication side effects (dizziness, confusion, falls, constipation)
- Pain levels and any new or spreading symptoms
Use a journal or phone app to record patterns—this data helps your doctors make better treatment decisions.
CRPS Suicide Prevention: Crisis Resources
CRPS is sometimes called “The Suicide Disease” because of the severe, unrelenting pain many patients experience. If you are experiencing thoughts of suicide or self-harm, please reach out immediately:
- National Suicide Prevention Lifeline: 988 (call or text, 24/7)
- Crisis Text Line: Text HOME to 741741
- International Association for Suicide Prevention:https://www.iasp.info/resources/Crisis_Centres/
You are not alone, and help is available.
Conclusion: Living With CRPS Long-Term
CRPS itself won’t shorten your life, but ignoring secondary risks can. The research is clear: proactive management of mental health, cardiovascular health, and mobility makes a measurable difference in outcomes.
Your next steps:
- Schedule a mental health screening if you haven’t had one in the past 6 months
- Request a cardiovascular evaluation at your next appointment, especially if you experience heart rate fluctuations
- Review your medications with your doctor to identify any unnecessary risks
- Start tracking symptoms weekly using the checklist above
- Connect with a CRPS support community like RSDSA for peer support and resources
With proper monitoring and comprehensive care, people with CRPS can and do live full, meaningful lives.
Frequently Asked Questions
Is CRPS a Permanent Disability?
CRPS can be a long-term or permanent condition for some individuals, but with early treatment, pain management, and rehabilitation, many can improve and regain function over time.
What Is the Final Stage Of CRPS?
The final stage of CRPS, often referred to as “atrophic,” can involve severe, irreversible changes, including muscle atrophy, joint stiffness, skin changes, and significant loss of function in the affected limb.
Is CRPS Considered a Terminal Illness?
No, CRPS is not considered a terminal illness. While it can cause significant pain and disability, it is not directly life-threatening. The main risks come from secondary complications, not the condition itself.
What Not to Say to Someone With CRPS?
Avoid saying things like “You look fine,” “It’s all in your head,” “Just push through it,” or “You should be better by now.” These dismiss their pain and struggles.
What Does CRPS Do to Your Heart?
CRPS can affect the heart by causing autonomic dysfunction, which can lead to symptoms such as a rapid heart rate, blood pressure fluctuations, and poor circulation. These changes can increase cardiovascular risk over time.








