If you have been dealing with brain fog, chronic fatigue, sinus congestion, or mood changes that no doctor can fully explain, mold exposure could be the missing piece.
Mycotoxins produced by indoor mold do not just irritate your lungs. Research shows they can accumulate in fatty tissues, disrupt your immune system, and recirculate through your body for months after the initial exposure ends.
The challenge is that most online advice on mold detox offers scattered tips without a clear sequence, and the order you follow matters more than most people realize.
This guide walks you through a structured, evidence-based 5-phase recovery protocol, from removing the source to rebuilding your health, backed by peer-reviewed research and clinical frameworks used by environmental medicine specialists.
What Is Mold and Why Does It Make You Sick?
Mold is a type of fungus that grows wherever moisture, warmth, and organic material exist together. While it plays a natural role in breaking down dead matter outdoors, it becomes a health concern when it colonizes indoor spaces and releases harmful compounds into the air you breathe.
How Mold Enters Your Body
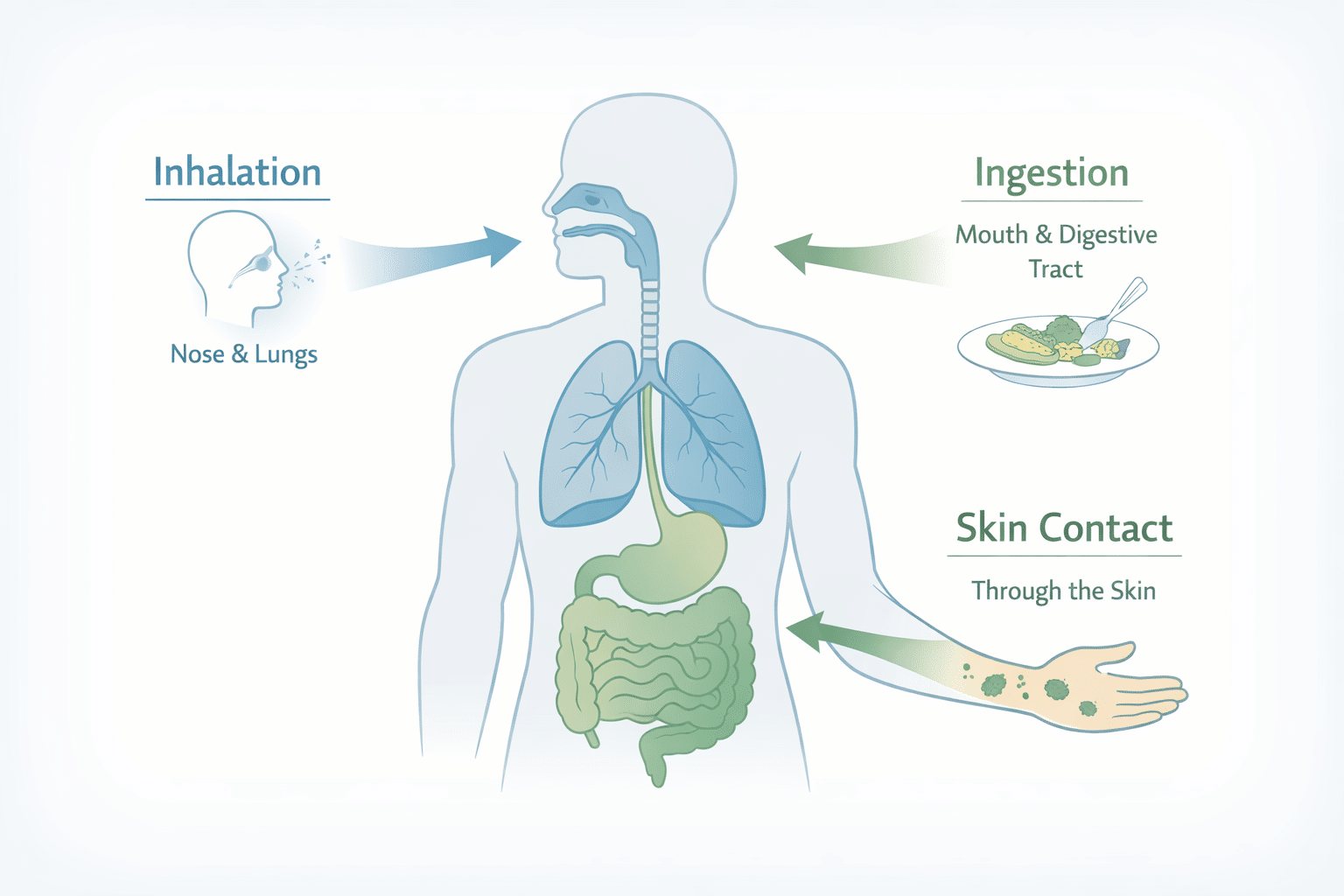
Mold reaches your body through three routes. Inhalation is the most common. Every breath you take in a room with active mold growth draws in microscopic spores and volatile compounds.
The CDC confirms that exposure to damp, moldy environments can cause stuffy nose, throat irritation, coughing, wheezing, and more severe reactions in people with asthma or weakened immune systems.
Ingestion happens when you consume mycotoxin-contaminated foods like stored grains, nuts, dried fruits, or coffee. Skin contact with mold-contaminated surfaces can also trigger localized rashes and irritation.
One distinction worth understanding: mold spores and mycotoxins are not the same thing. Spores are the reproductive “seeds” mold uses to spread.
Mycotoxins are toxic chemical byproducts that certain mold species produce under specific conditions. Mycotoxins are far smaller, can penetrate deep into tissues, and are responsible for the more severe systemic symptoms.
Common indoor mold species include Aspergillus, Penicillium, Cladosporium, and Stachybotrys (black mold).
What Is Black Mold?
Black mold typically refers to Stachybotrys chartarum, a slow-growing species that thrives on cellulose-rich materials like drywall and wood in high-moisture environments. However, not every dark-colored mold is Stachybotrys, and not every Stachybotrys colony actively produces mycotoxins.
According to Harvard Health, black mold does not appear more dangerous than other indoor mold types based on current evidence. Dr. Nicholas Nassikas of Harvard Medical School notes that prolonged exposure to any indoor mold may contribute to respiratory problems, lung inflammation, and cognitive changes.
A growing body of functional medicine research suggests prolonged mycotoxin exposure may contribute to Chronic Inflammatory Response Syndrome (CIRS) in genetically susceptible individuals.
A peer-reviewed literature review published in PMC concluded that CIRS is an inflammatory illness affecting multiple body systems, and the Shoemaker Protocol remains the only treatment with documented clinical efficacy. The takeaway: do not panic over mold color, but take all indoor mold growth seriously.
Why Some People Get Sicker Than Others?
Research into HLA-DR gene variants shows that roughly 25% of the population carries genetic markers associated with reduced ability to clear biotoxins.
If you carry these variants, your immune system may fail to tag mycotoxins for removal, allowing them to recirculate and trigger ongoing inflammation. Other risk factors include a compromised immune system, pre-existing respiratory conditions, and autoimmune disease history.
This genetic variability explains why one person in a household can be severely affected while others show no symptoms.
Mold Exposure Symptoms You Should Not Ignore
Mold exposure rarely announces itself with one clear symptom. Instead, you may notice a cluster of seemingly unrelated complaints spanning multiple body systems.
Respiratory and Sinus Symptoms
Chronic congestion, sinus pressure, postnasal drip, wheezing, shortness of breath, and a persistent cough are the most widely documented signs.
The Institute of Medicine’s report found sufficient evidence linking damp indoor spaces to upper respiratory symptoms and asthma. A 2007 meta-analysis estimated that home dampness raises asthma-related risks by 30 to 50%.
Neurological and Cognitive Symptoms
If you are experiencing brain fog, memory lapses, difficulty concentrating, or word-finding trouble, mycotoxin exposure deserves consideration.
A 2020 study by Harding et al. in Brain, Behavior, and Immunity demonstrated that mold inhalation triggered innate immune activation along with cognitive and emotional dysfunction in controlled animal models. Earlier clinical research found cognitive impairment patterns similar to mild traumatic brain injury in 182 mold-exposed patients.
Fatigue, Pain, and Mood Changes
You may notice deep, unrelenting exhaustion that sleep does not resolve, joint and muscle pain without clear cause, and mood shifts including anxiety, depression, and irritability.
A review of 19 studies cited by Harvard Health found that prolonged mold exposure increased stress, depression, and anxiety in both adults and children.
A Brown University study of nearly 6,000 adults found that residents of damp, moldy homes had 34 to 44% higher depression risk.
Gut and Skin Symptoms
New food sensitivities, bloating, alternating constipation and diarrhea, unexplained rashes, and hives can all result from mycotoxin damage to the gastrointestinal lining and skin. The EPA notes that skin rash is among the recognized allergic responses to mold.
How Mold Affects Your Body
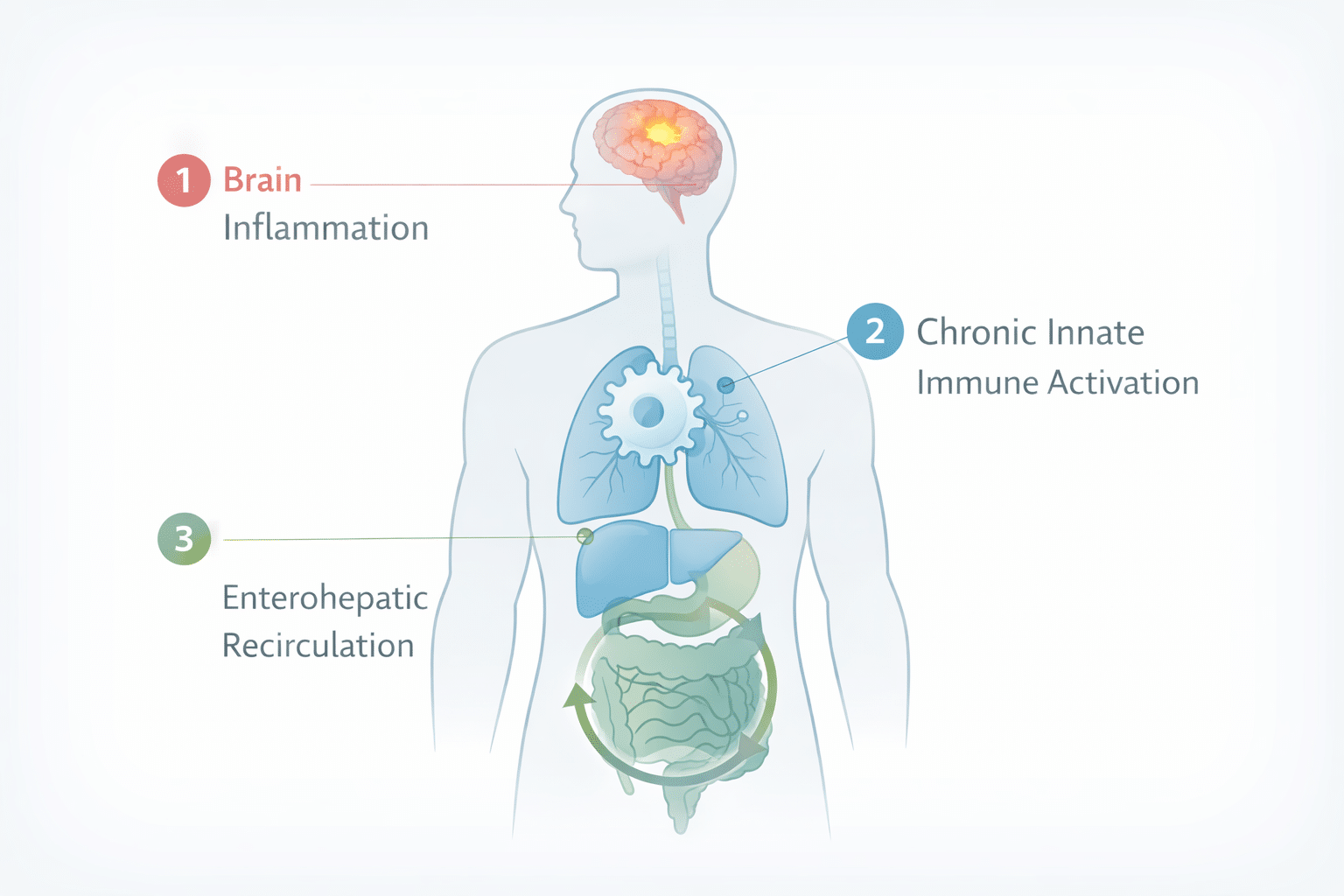
The Mycotoxin Problem
Mycotoxins are fat-soluble, meaning they accumulate in fatty tissues including the brain and liver.
They also recirculate through your enterohepatic pathway: the liver packages them into bile, the bile enters the gut, and roughly 95% gets reabsorbed back into the bloodstream.
Without intervention to break this cycle, symptoms can persist long after you leave the moldy environment.
Immune System Disruption
Mold triggers chronic innate immune activation, which shows up as elevated inflammatory markers like C-reactive protein, TGF-beta, MMP-9, and C4a.
Your innate immune system stays overstimulated while your adaptive immunity may become suppressed, creating a state of simultaneous inflammation and vulnerability. This dysregulation can also activate mast cells, leading to histamine-related symptoms.
Liver and Detox Pathway Overload
Your liver processes toxins through Phase I (breakdown) and Phase II (conjugation for excretion) pathways. The two Phase II pathways most critical for mycotoxin clearance are glutathione conjugation and glucuronidation.
When these pathways are overwhelmed, mycotoxins recirculate, glutathione levels drop, and oxidative stress climbs.
How to Detox From Mold: A 5-Phase Recovery Protocol
Recovering from mold is a sequence, not a single action. The order matters because skipping steps often causes setbacks.
Phase 1: Remove the Source
You cannot detox while still being exposed. Inspect your home for visible mold, water damage, and musty odors. Check bathrooms, basements, HVAC systems, and behind drywall.
Keep humidity below 50% with dehumidifiers, run HEPA air purifiers in sleeping areas, and follow EPA guidance: if the affected area exceeds 10 square feet, hire professional remediation. ERMI or HERTSMI-2 testing provides comprehensive environmental assessment.
Phase 2: Test Your Toxic Load
Urine mycotoxin panels (RealTime Labs, Mosaic Diagnostics) measure your current mycotoxin burden. Blood markers like TGF-beta, MMP-9, C4a, and VIP reveal immune activation levels. Visual Contrast Sensitivity testing offers an accessible screening tool.
HLA-DR genetic testing identifies whether you carry susceptibility variants. Testing guides your protocol rather than leaving you guessing.
Phase 3: Open Drainage Pathways
This is the step most people skip, and it causes the most problems. Using binders before your elimination pathways are functioning can redistribute toxins and worsen symptoms.
Ensure at least one daily bowel movement with magnesium citrate, fiber, and hydration. Support lymphatic flow through dry brushing, rebounding, and regular movement.
Support your liver with milk thistle, dandelion root, NAC, and glutathione precursors. Use nasal irrigation for sinus clearance and consider infrared sauna sessions (with practitioner approval) for toxin elimination through sweat.
Phase 4: Introduce Binders
Once drainage is established, binders attach to mycotoxins in the gut and prevent reabsorption. Start gentle: Saccharomyces boulardii, chlorella, or modified citrus pectin.
Progress to moderate options like activated charcoal, bentonite clay, or zeolite. Prescription binders such as cholestyramine are reserved for severe cases under medical supervision.
Take binders 1 to 2 hours away from food and medications. Start low and increase gradually to avoid Herxheimer reactions.
Phase 5: Rebuild and Restore
Replenish glutathione with liposomal forms. Rebuild your gut microbiome with multi-strain probiotics containing Lactobacillus and Bifidobacterium strains.
Dr. Michael Ruscio notes that certain probiotics may also bind mycotoxins and reduce absorption. Restore depleted nutrients (vitamin D, zinc, omega-3s, B vitamins), support mitochondrial function with CoQ10 and alpha-lipoic acid, and retest mycotoxin levels every 3 to 6 months.
How to Detox From Mold Exposure Naturally
The clinical protocol above gives you the medical framework. But your daily food and lifestyle choices form the practical foundation of recovery. These strategies work for anyone dealing with mold exposure, even before you see a specialist.
Anti-Inflammatory and Low-Mold Diet
What you eat during a mold detox either supports or undermines your progress. The goal is simple: lower inflammation and stop reintroducing mycotoxins through food.
Foods to eat during mold detox:
| Category | What to Include | Why It Helps |
|---|---|---|
| Vegetables | Broccoli, cauliflower, kale, asparagus, Brussels sprouts, bell peppers | Cruciferous types contain sulforaphane, which supports Phase II liver detox |
| Low-sugar fruits | Berries, green apples, lemons, limes, avocado | Provide antioxidants without feeding fungal overgrowth |
| Clean proteins | Wild-caught fish, grass-fed meat, pasture-raised eggs | Supply amino acids for tissue repair and immune function |
| Healthy fats | Olive oil, coconut oil, avocado oil, ghee | Support cell membranes and anti-inflammatory signaling |
| Anti-fungal foods | Garlic, ginger, turmeric, onions | Contain natural anti-fungal and anti-inflammatory compounds |
| Gut support | Bone broth | Repairs gut lining and supports liver function through glycine |
Foods to avoid during mold detox:
| Category | What to Remove | Why It’s Harmful |
|---|---|---|
| Sugar and refined carbs | White bread, pastries, candy, soda | Feed fungal overgrowth directly |
| High-mycotoxin grains | Wheat, corn, and corn-based products | Among the most common mycotoxin carriers in the food supply |
| Histamine triggers | Aged cheeses, fermented foods (kimchi, sauerkraut, kombucha) | Can spike histamine reactions during active detox |
| Mold-contaminated foods | Dried fruits, peanuts, pistachios | Carry high mold contamination risk due to storage conditions |
| Alcohol | All types | Impairs liver function and promotes fungal growth |
| Coffee | Conventional brands | Common mycotoxin source unless the brand tests for mold |
| Mushrooms | All varieties during active detox | Fungal source that can aggravate symptoms |
How Long Does Mold Detox Take?
This is the question everyone asks, and the honest answer is: it depends. There is no universal timeline because the variables that determine recovery speed are highly individual.
| Exposure Severity | Typical Recovery Timeline | Description |
|---|---|---|
| Mild Exposure | A few weeks to 2 months | Occurs in individuals without genetic susceptibility. Once exposure is removed and basic supportive measures are implemented, symptoms often resolve relatively quickly. |
| Moderate Exposure | 3 to 6 months | With a consistent recovery protocol, most individuals experience meaningful improvement during this timeframe, though complete recovery may take longer. |
| Severe or Prolonged Exposure | 6 months to 2+ years | More common in individuals with HLA-DR gene variants that impair biotoxin clearance. Recovery may take significantly longer due to the body’s reduced ability to eliminate toxins. |
When to See a Professional?
Seek professional guidance if your symptoms are severe or worsening, you suspect internal mold colonization, you have an autoimmune condition or compromised immunity, or you have been symptomatic for over 6 months without improvement. Look for practitioners trained in the Shoemaker Protocol, CIRS treatment, or environmental medicine. Most conventional physicians are not specifically trained in mold toxicity, so a functional medicine or integrative practitioner with mold experience is often more appropriate for this condition.
Conclusion
Mold detox is not a weekend cleanse or a single supplement fix. It is a phased, methodical process that begins with removing the source, continues through testing, drainage support, and targeted binder use, and ends with restoring the systems that mold exposure compromised.
Your timeline will depend on variables like exposure duration, genetic susceptibility, and how consistently you follow each phase.
If you are experiencing persistent symptoms across multiple body systems, do not dismiss the possibility that your environment is the root cause.
Work with a practitioner trained in CIRS or environmental medicine, test before you guess, and give your body the structured support it needs to recover fully.








